Five Reasons for the Explosive Increase in Gluten Reactions (and Buttermilk Buckwheat Pecan Pancakes)
Last Updated September 26, 2017 · First Published October 14, 2012
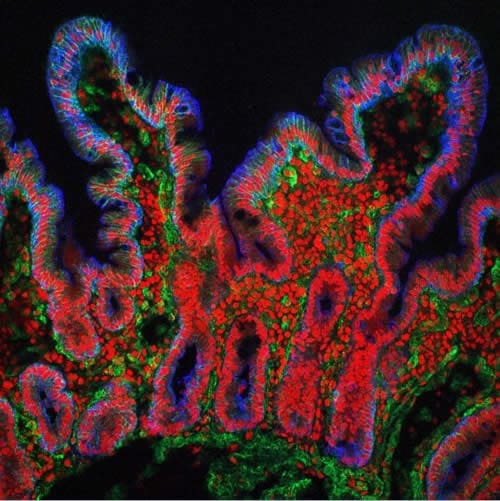
Like the proverbial canary in a coal mine, Gluten-Reactive people are showing us the problems with highly processed foods, especially wheat, rye, and barley.
“Auto-immune inflammatory damage, villous atrophy of the small intestine” test results is currently considered the diagnostic criteria for celiac disease.
What are villi? The tiny absorptive fingers of our gastrointestinal (GI) tract, that become damaged and broken off without regrowth. This is the diagnostic criteria for celiac disease. Autoimmune damage has been escalating in people since the 1950s.
Gluten reactivity: Any change in function due to gluten ingestion that isn’t demonstrated by villous atrophy. Some typical symptom include gas, bloating, migraines, menstrual irregularities, and brain fog.
Why the rapid rise in Gluten intolerance? Our bodies haven’t changed genetically as quickly as our environment has changed.
1. The SAD Diet
We have moved from a grazing diet of plants with some meat protein, fruits, and nuts in season to a Standard American Diet (SAD) of primarily highly processed wheat, multiple times per day. Lacking the fiber or nutrition of whole grain, we combine it with other highly processed starches, highly processed meat, and vast quantities of sugar.
2. Sugar
Our bodies are genetically able to handle a certain amount of concentrated sugar, a larger amount of fats, an even larger amount of fiber. Our current diet turns the concentrations topsy-turvy. Every bit of that excess sugar is damaging our intestinal tract through inflammatory changes. Even the “natural” food companies use highly concentrated syrups of grains to balloon the sugar content.
3. Chemical Exposure
Environmentally, exposure to so many chemicals daily that didn’t even exist two generations back has escalated the damage to our bodies. Chemical irritants like BPA (bisphenol A) in cans and plastics, inorganic Arsenic compounds from insecticides used in the 1950s, pesticides, herbicides, sodium lauryl sulfate (a foaming agent contained in most shampoos), toothpastes and soaps, and non-steroidal anti-inflammatories like Aspirin all increase the likelihood of intestinal irritation.
Each of these exposures create inflammatory changes in our mucosa, allowing intact proteins to be absorbed into our bloodstreams. Intact proteins in the bloodstream provoke high-level reactivity within the bloodstream. Our immune system goes into overdrive to rid itself of these intruders. Over time, this pattern of reactivity can lead to an autoimmune response, breaking down our own tissue instead of the intruder.
4. Genetic Manipulation
Wheat has morphed from kernels of 14 genes to 42 genes count with many genetic variations in morphology. No longer a tall, low-carbohydrate/high-fiber grain, now it is a short, high-carbohydrate, lower-fiber weak plant that is easily harvested.People don’t genetically change that quickly.
It takes thousands of years for genetic changes to adapt to external environmental changes. The variation in fiber content especially changes our gut bacteria.
5. Bacteria
We’ve lost our happy, beneficial commensal bacteria in part because we’ve lost the fiber that fed them over time, lost some of the microbiome that create vitamin B-12 from foods we ingest, and decreased those bacteria that are protective in the ongoing fight for our health. When the bacteria inside our bodies are so different from the ideal conditions, our gut changes, and inflammation occurs. Studies have shown that the bacterial colonization of the typical gluten-reactive person is vastly different from a non-reactor.
What to do to keep ourselves healthy?
Avoid Gluten. Yes, all of us would do well to avoid highly processed wheat, rye, and barley. Even for the non-gluten-sensitive, eating grains multiple times per day is just not healthy.
Repair the gut, using real foods high in glutamine. Feel free to use tasty ones like sauerkraut, meat, and dairy. If possible use only organically grown to avoid the chemical additions.
Increase beneficial bacteria using live foods. Yogurt is not the only source of terrific bacteria, consider miso, kimchi and other pickles. By increasing your diversity of internal bacteria, you will strengthen your immunity.
“Villi from the small intestine” © 2011 S. Schuller, Wellcome Images, used under Creative Commons license.
























Great post! As a personal chef that specializes in healthy cooking (I lost over 100 lb several years ago going unprocessed and mainly gluten free) I have a lot of gluten free clients. I get people from time to time asking why I promote gluten free recipes to those that don’t have Celiac disease, so I will keep this post to refer them to! I experienced a better quality of life going gluten free the majority of the time, as well as every single personal chef client that has switched to a gluten free lifestyle….and it wasn’t all in our head. 😉 Thank you again!
Glad I could give you a good citation. 🙂
The pancakes look delicious! Can’t wait to make them for my little one!
Glad to hear you continue to explore food reactions. Testing can be so important for initial diagnostics. Elimination and Challenge can then be used to fine tune the foods that aren’t perfect for you.
Thank you for this post, Jean. I’m so glad it was included in October Unprocessed. I have Celiac (self-diagnosed, went gf instead of doing tested) and have been gf for over 2 1/2 years. My life-long issues that were separately diagnosed all resolved once my body was free of gluten and I’ve been able to manage my hypothyroid without any supplements to support it (Synthroid made me worse).
I have since gone dairy-free (last year) and egg-free (last month) after noticing reactions.
With the drastic change in my health since going gf, I always urge friends and family to get tested for food allergies and intolerances when when everything else they are tested for comes up negative and they aren’t getting answers. I’m still trying to get family members to get tested. 😀
I love this blog post! I have had a very similar hypothesis about the rise in gluten intolerance since I became gluten intolerant. I had always felt good enough growing up, but I lived abroad in Europe for 4 months (eating tons of baguettes and cheese) and when I got back, both American gluten and dairy made me sick. I am now able to process goat and sheep dairy and raw imported cow dairy, however I can no longer process American gluten. I loved how elegantly you put this into words.
Thanks for all the compliments, very flattered.
I have many patients who “cheat” while on vacation in Europe without seeing any reactions. Makes me wonder about the other differences there are in cultivation practices.
Our family just finished up two weeks of going gluten-free. None of us are sensitive to gluten, our main reason for doing it was to expand our knowledge of other foods such as buckwheat, quinoa, amaranth and millet….along with the realization that to eat wheat everyday simply could not be good for us in the long run. Realistically we began consuming wheat again today (as our budget allows for) – yet it is our goal to have a more healthy mix of gluten days and gluten free days. I am not sure how much of the wheat is hybrid where we live in Hungary. Just 5 years ago we grew our own wheat, rye and barley and we had the chance to eat our own grains which was a wonderful experiment as well. So while non of us felt “better” eating gluten free, I do know people whom it affects… Read more »
Isn’t it wonderful when you finally figure out what is making you ill?
Great post…I wrote about some of this on my blog a couple of days ago! I think it’s a shame that many people who don’t have celiac disease complain that gf is a fad, instead of understanding that it’s possible we’d all be better off with less gluten (and certainly less wheat) in our diets.
Hi Winnie,
Great minds bring about the great changes. Now I need to click through to link with you.
I agree that it would behoove us to reduce the amount of wheat, rye and barley consumed by all of us.
I have been gluten free since January and feel better than ever. I no longer deal with frequent stomach issues, my skin is better, my allergies are dramatically improved, and I don’t have the joint pain I once had. Now if I could just get my husband and kids to fully convert … that is my current challenge.
Hi Jennifer,
I’ve found the positive changes in you will be the reason your husband and children will change. Nothing like seeing someone you love feeling better to inspire.